Autoimmune diseases Part 2: Disease modifying treatments and monitoring
Dr Gerry Morrow
Dr Gerry Morrow
MB ChB, MRCGP, Dip CBT
Medical Director Clarity Informatics
Editor Clinical Knowledge Summaries
Practice Nurse 2021;51(7):30-34
Last time we looked at the signs and symptoms of, and investigations used to diagnose, common autoimmune diseases. In part 2, we describe the function and effects of disease modifying treatments, a practical approach to shared monitoring and a referral strategy for those who may need specialist care
In the absence of treatment, autoimmune diseases can cause wide-ranging and severe end-organ damage. Before the advent of disease modifying treatments people with systemic lupus erythematosus (SLE), rheumatoid arthritis, and other arthritides had deeply unpleasant experiences and difficult-to-control symptoms, such as joint deformities, skin lesions, renal failure, and complex heart disease.1
Disease modifying treatments, with continued administration, have provided an invaluable lifeline and, in some people, a curative approach. That said, these are powerful drugs with potentially powerful adverse effects.
HOW DISEASE MODIFYING ANTIRHEUMATIC DRUGS WORK
Disease modifying antirheumatic drugs (DMARDs) can be classified into two broad categories; conventional and biological treatments – the ‘biologics’.2
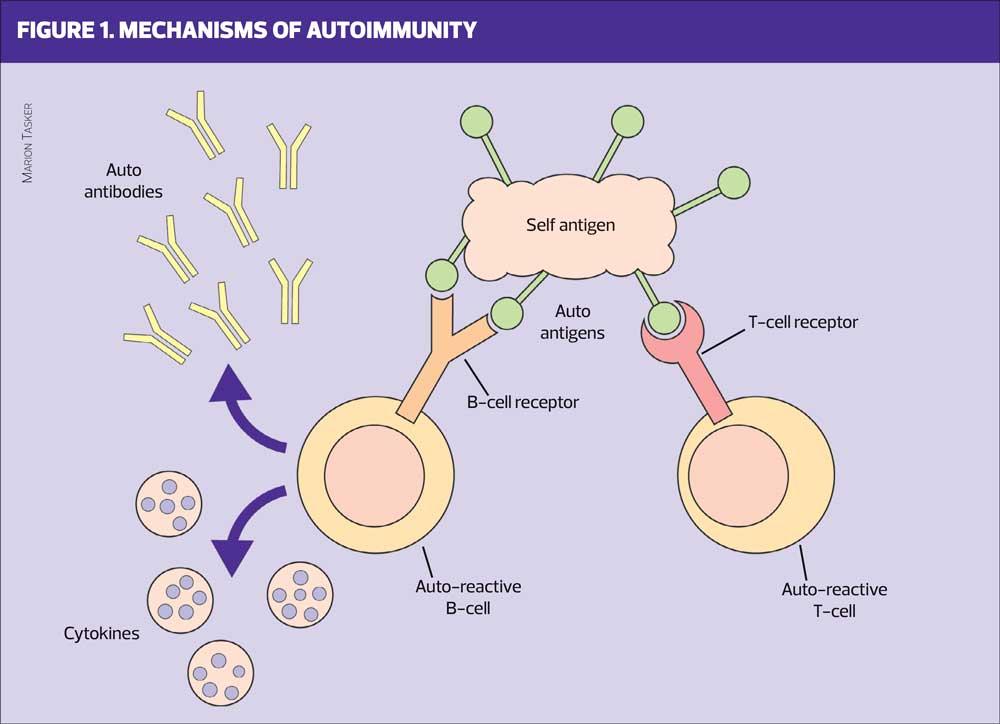
Conventional DMARDs, such as methotrexate, work in a variety of ways, including the suppression of production of cytokines, such as interleukins. These interleukins are produced by white blood cells and help drive inflammation.3
Biological DMARDs have a different mode of action. They also act on interleukins but, additionally, appear to directly affect T helper cells and neutralise tumour necrosis factors. They therefore have a broader effect on autoimmune disease.4
Given that these treatments have an impact on the immune system and are prescribed to suppress some elements, it is possible that this suppression can, in some people, lead to the development of some unusual infections, including tuberculosis, fungal infections, and listeria. The reason for these infections is often related to lower white cell counts, which is why this is part of the regular monitoring of treatment.
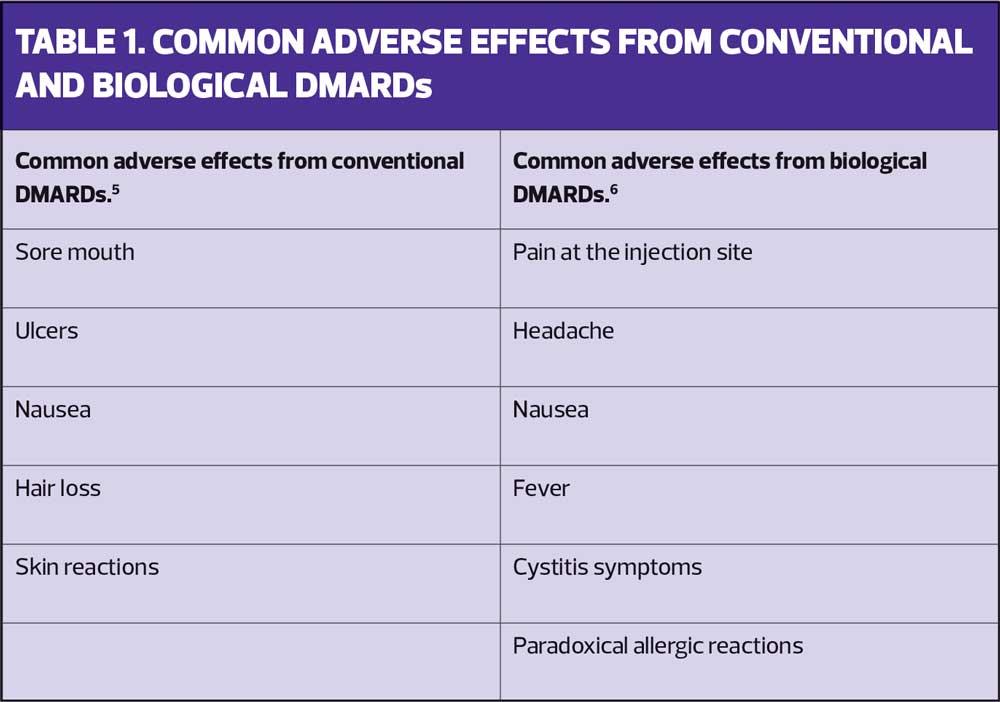
Table 1 lists the common adverse effects of conventional and biological DMARDs.
PRINCIPLES OF DISEASE MODIFYING TREATMENT
Eligibility criteria
First, we need to understand who is prescribed which medications for autoimmune diseases. Once a diagnosis has been made specialists will initiate a disease modifying agent, to tackle not just the symptoms but to halt the progress of inflammation and organ damage. The usual first line, oral, conventional DMARDs include:
- Methotrexate
- Leflunomide
- Sulfasalazine
- Azathioprine
- Penicillamine
- Hydroxychloroquine.7
Many people will respond to their first drug, but a significant number will suffer unacceptable side effects or simply not respond and are therefore moved to a second DMARD.
Failure to respond to a second DMARD usually results in consideration of a biological therapy (usually injectable). Part of this decision is based on the severity scores that form part of the assessment of most people with autoimmune diseases.7
The commonly used severity score in rheumatoid disease is called DAS28.8 In psoriatic arthropathy the severity score is PASI,9 and in ankylosing spondylitis ASDAS.10 For each of these the score is determined using a composite of disease indicators and inflammatory markers. The scores can also be used to monitor disease progression. Usually this scoring is undertaken in a hospital setting and can be used as a threshold to determine eligibility for newer, costly, biological treatments.
PRESCRIBING AND MONITORING
Prescribing DMARDs is always part of a shared-care protocol. Treatment and initial monitoring are usually carried out by a specialist in secondary care.8 Local shared care protocols should have outlines to provide guidelines on referral criteria and access to services for urgent patient needs.
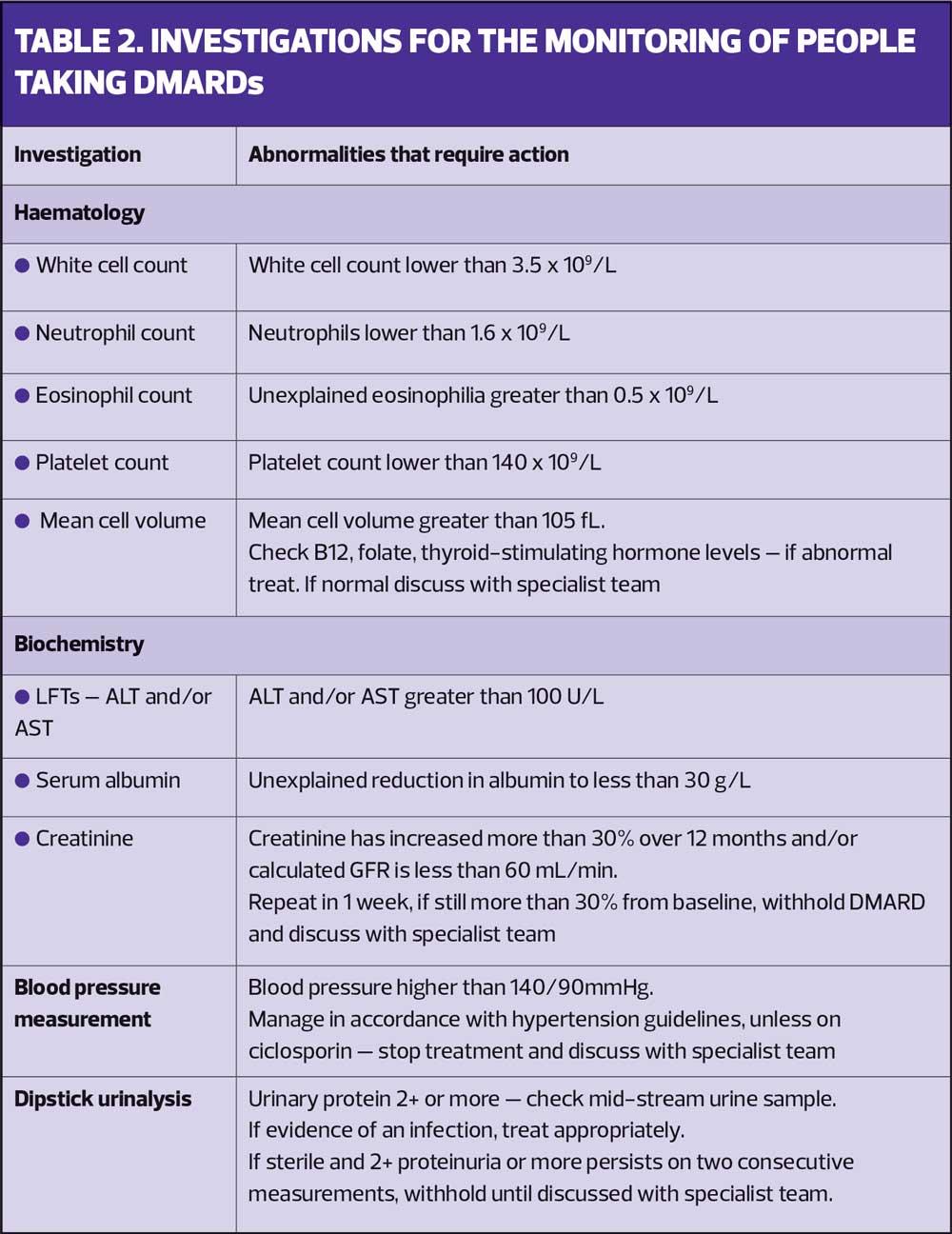
Once the person is stabilised on treatment, the practice may be asked to prescribe and monitor therapy and this role may be devolved to practice nurses. In this role you will need to monitor the person's health and liaise with their specialist team, particularly regarding any complication of therapy or disease flares. It is vital that monitoring follows local guidelines and protocols, particularly in respect of the areas in Table 2. Table 2 lists the routine monitoring of blood values, and other markers, and the appropriate action in the case of an abnormality being detected.
Infection
People taking DMARDs are more prone to infection, especially in the first 6 months of treatment. You should therefore advise the person to avoid contact with people who have shingles or chickenpox. If they come in to contact with these people, they must seek urgent medical advice.1
Additionally, people taking DMARDs are also at higher risk of increased morbidity and mortality from COVID-19 infection. Most were advised to shield in the first wave of the pandemic and were identified as a high priority group for vaccination. Early research on COVID vaccine-related immunity in this group has shown benefits similar to those individuals not on DMARDs.
Major toxicity
You will need to be alert to any adverse effects related to the DMARD which might present. Major toxicity with DMARDs can occur during intercurrent illness, particularly if a person has impairment of renal function or sepsis. Should this happen, you will need to seek specialist advice as treatment may need to be temporarily discontinued.
Drug interaction
The prescription of medicines which have the potential to interact with DMARDs must be avoided.1,8 If you are a prescriber, you should consult the British National Formulary (BNF) or the relevant summary of product characteristics.
Vaccination
As a matter of routine, these individuals should be offered vaccinations to prevent the serious infections that are more common in people exposed to DMARDs. This includes annual influenza vaccine and a pneumococcal vaccine, preferably before starting the DMARD. Pneumococcal vaccine should be repeated at 10-yearly intervals if given before starting the DMARD, or at 5-yearly intervals if given after starting it.1,8
Live vaccines (e.g. yellow fever and rubella) are contraindicated. You should always seek specialist advice if a live vaccine is being considered.
All currently licensed COVID vaccinations are appropriate for individuals who are receiving DMARDs and/or biologics. There is however, some limited evidence that the efficacy of some vaccines may be reduced for people receiving these treatments.
Patient information
Ensure that people on DMARDS have been provided with suitable medicines information leaflets and are aware of potential adverse effects. They should also be provided with information about who to contact if these should develop, particularly a direct connection to their specialist team when appropriate.
SPECIALIST REFERRAL
For people on any DMARD, practice nurses should consider stopping treatment and referring urgently to the person’s specialist if monitoring results show any of the abnormalities listed in Table 2.1,8
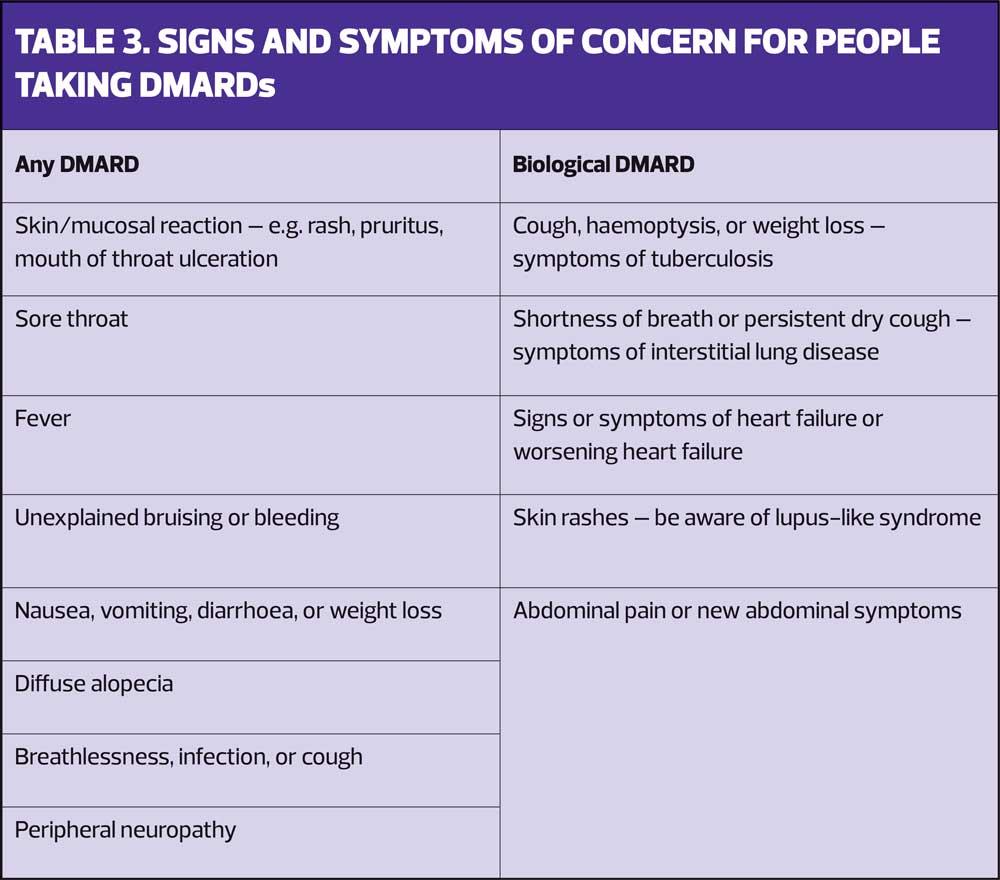
In addition consideration should be given to stopping treatment and referring urgently to rheumatology should any of the signs or symptoms listed in Table 3 develop.1,8
THE ROLE OF THE PRACTICE NURSE
The role of practice nurses is as part of the multidisciplinary team managing people with autoimmune diseases and, as such, to ensure that the person has rapid access to specialist care for flares, including information about when and how to access this care. For example, check the person has a named rheumatology specialist nurse who coordinates care, and has access to physiotherapy, occupational therapy, and podiatry services for advice on mobility, pain control, work-related issues, and foot health.
Practice nurses also have a role in offering an annual review, regular medication reviews and regular drug monitoring at appropriate intervals, depending on the person, the local protocol and the drug(s) being administered.
You should also assess disease activity and damage, and measure functional ability (using, for example, the Health Assessment Questionnaire [HAQ]).11 In this way you can assess the effect the disease is having on the person's life.
Practice nurses are also well placed to check for the development of comorbidities, such as hypertension, ischaemic heart disease, osteoporosis, and depression. You should assess symptoms that suggest complications, such as vasculitis and disease of the cervical spine, lung, or eyes.
It is important to recognise when monitoring people on DMARDs that, although absolute values of serum blood test levels are useful indicators, trends are equally important. Any rapid fall or rise, or a consistent downward or upward trend in any parameter warrants extra vigilance; e.g. gradual decreases in white blood cells or albumin, or increasing liver enzymes.1,8
It is also important to note that people who are on one DMARD are likely to be taking a second (e.g. methotrexate or sulfasalazine), or even a third medication. Monitoring frequency for people on more than one DMARD should be based on the DMARD which requires the most frequent monitoring.
SUMMARY
Practice nurses have a key role to play in the multidisciplinary team management of people with autoimmune disease, their ongoing treatment and monitoring. As part of this responsibility it is important to understand the range of potential adverse effects, varying blood parameters and signs that people on DMARDs might present with during chronic disease monitoring. Local shared care protocols should provide guidelines on referral criteria and access to services for urgent patient needs and you will need to be aware of these.
The increasing prevalence of autoimmune diseases, new developments in treatment and DMARDs and their wider usage means that you will find that more people are being prescribed these drugs. Inevitably this will result in the take up of a greater percentage of time for primary care chronic disease management. However, it is imperative that increasing pressure does not result in the monitoring of these individuals becoming a ‘tick box’ exercise. The consequences of poor monitoring are serious – for both the affected individual and the health service.
REFERENCES
1. NICE Clinical Knowledge Summaries. Rheumatoid Arthritis; 2020 https://cks.nice.org.uk/topics/rheumatoid-arthritis/background-information/complications/
2. Rosenblum MD, Gratz IK, Paw JS, et al. Treating human autoimmunity: current practice and future prospects. Sci Tral Med 2012; 4(125), 125sr1 https://doi.org/10.1126/scitranslmed.3003504
3. Cutolo M, Sulli A, Pizzorni C, et al. Anti-inflammatory mechanisms of methotrexate in rheumatoid arthritis. Ann Rheum Dis 2001;60(8):729-735. https://ard.bmj.com/content/60/8/729
4. Billmeier U, Dieterich W, Neurath MF, et al. Molecular mechanism of action of anti-tumor necrosis factor antibodies in inflammatory bowel diseases. World J Gastroenterol 2016; 22(42): 9300-9313 PMID: 27895418 DOI: 10.3748/wjg.v22.i42.9300 https://www.wjgnet.com/1007-9327/full/v22/i42/9300.htm
5. John M. Eisenberg, Center for Clinical Decisions and Communications Science. Medicines for Rheumatoid Arthritis: A Review of the Research for Adults. 2012. Possible Side Effects of DMARDs. https://www.ncbi.nlm.nih.gov/books/NBK115126/table/consra2.tu1/
6. NICE British National Formulary; 2021 https://bnf.nice.org.uk/drug/etanercept.html#sideEffects
7. NICE Pathways. Drug Treatment for rheumatoid arthritis; 2021. https://pathways.nice.org.uk/pathways/rheumatoid-arthritis#path=view%3A/pathways/rheumatoid-arthritis/drug-treatment-for-rheumatoid-arthritis.xml&content=view-index
8. NICE NG100. Rheumatoid arthritis in adults: management; 2020. https://www.nice.org.uk/guidance/ng100/
9. British Association of Dermatologists. Guidelines for biologic therapy for psoriasis; 2017. https://www.bad.org.uk/shared/get-file.ashx?id=5835&itemtype=document
10. Pedersen SJ, Sørensen IJ, Garnero P, et al. ASDAS, BASDAI and different treatment responses and their relation to biomarkers of inflammation, cartilage, and bone turnover in patients with axial spondyloarthritis treated with TNFα inhibitors. Ann Rheum Dis 2011;70:1375-1381. https://ard.bmj.com/content/70/8/1375
11. RheumInfo. Health Assessment Questionnaires. https://rheuminfo.com/physician-tools/health-assessment-questionnaires-haq-haq-ii-mdhaq/
Related articles
View all Articles