Lower targets set for 2016-17 winter flu campaign
Mandy Galloway
Mandy Galloway
Editor, Practice Nurse and medical writer
Lower targets across most eligible groups for the coming seasonal flu campaign should make it more feasible to achieve them - but practice nurses are still in for a busy time ahead
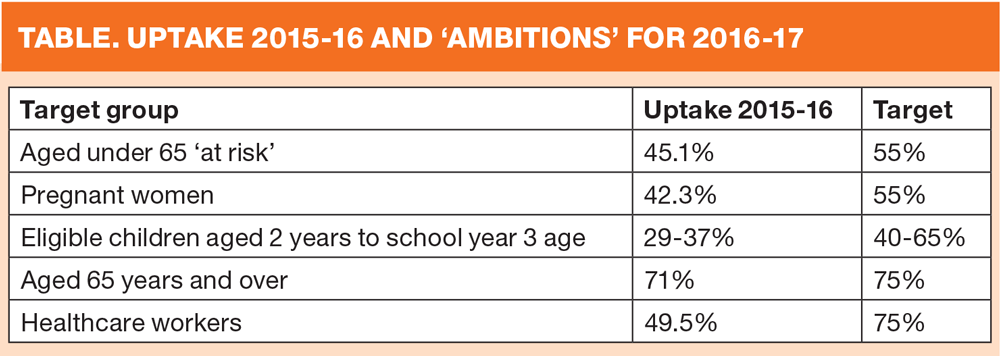
Practices have been urged to aim for targets of between 40% and 75% for all eligible groups for this year’s seasonal flu campaign after previous, more ambitious targets were missed.
In recent years, the target has been 75% across the board, but uptake has been falling. The seasonal flu campaign in 2014-15 was undermined by reports that the vaccine was not effective against some of the strains of flu in circulation, and last year’s mild winter may have lulled patients into a false sense of security.
Although Public Health England (PHE) has not made much noise about the lower targets for the coming season, they have been reduced substantially compared with previous years.
The most modest target is for children aged 2 years to school year 3 age – at 40-65%, after a ‘disappointing’ decline in uptake last winter compared with the first year that children were included in the target groups. PHE acknowledges both the ‘hard work of teams’ and that it can be challenging to reach pre-school children but says ‘reaching these pre-school cohorts continues to be extremely important for their own protection and to prevent the spread of flu.’
UPTAKE
Uptake in 2015-16 was down from 38.5% to 35.4% in 2-year-old children, from 41.3% to 37.7% in 3-year-olds, and from 32.9% to 30% in 4-year-olds. Uptake in the school-based programmes for older children was substantially higher, at over 50%. Results from 2014-15 showed that vaccinating children of primary school age resulted in a significant reduction in incidence for a range of indicators, including general practice consultations for influenza-like illnesses.
Last winter, more people than ever received a flu vaccination, but despite vaccinating greater numbers of patients, the percentages were lower. Uptake among the over-65s was 71%, down from 72.7% the previous year, and uptake for those aged 6 months to under 65 years in a clinical risk group was down from 50.3% in 2014-15 to 45.1% last season.
Uptake across all the risk groups was lower in 2015-16 than in 2014-15, despite the risk for people with long term chronic conditions becoming ‘very unwell’ from flu, and of being at significantly increased risk relative risk (RR) of flu-related death. Ironically uptake was lowest in patients with chronic liver disease (42.5%) who are at the greatest RR of flu-related death (48.2) compared with 11.3 RR for all at-risk patients.
More pregnant women were vaccinated against flu than the previous year – 305,478 compared with 286,156 in 2014-15. However the percentage dropped from 44.1% to 42.3% because there were greater numbers of eligible pregnant women. Pregnant women and their babies are at greater risk from the complications of flu, which is the most frequent single cause of death in pregnancy.
THE TARGETS
The target for vaccination of people in clinical risk groups (aged 2 – 65 years) is at least 55% of those eligible. Where a higher rate has been achieved in the past, this should be maintained.
For the over-65s, the target is 75% in line with the World Health Organization (WHO) target.
The other key group for whom the target is 75% is frontline clinical staff. Only half of this group was vaccinated last season. PHE reminds nurses that the NMC Code requires all registrants to ‘take all reasonable personal precautions necessary to avoid any potential health risks to colleagues, people receiving care and the public.’ While vaccination remains voluntary (unlike in other developed countries) all NHS staff (including nurses employed in general practice) are urged ‘to consider seriously the benefits to themselves and their family contacts, their patients and the NHS and, as a result, accept the offer of the vaccine.’ A practice nurse who has been vaccinated is in a strong position to encourage her patients to accept vaccination, and to dispel any myths – such as ‘the vaccine gives you flu’. It doesn’t.
THE VACCINE
For the 2016-17 flu season (northern hemisphere winter), WHO has recommended that trivalent vaccines contain the following strains:
- an A/California/7/2009 (H1N1)pdm09-like virus;
- an A/Hong Kong/4801/2014 (H3N2)-like virus;
- a B/Brisbane/60/2008-like virus.
It is recommended that quadrivalent vaccines containing two influenza B viruses contain the above three viruses and a B/Phuket/3073/2013-like virus.
One vaccine manufacturer, Sanofi Pasteur MSD has had a quadrivalent flu vaccine approved by the Medicines and Healthcare products Regulatory Agency (MHRA) but it is thought unlikely that it will be brought into use in the UK for the forthcoming season, although WHO includes quadrivalent vaccines in its recommendations. If quadrivalent rather than the usual trivalent flu vaccines had been used in the UK over the past decade, it is estimated that an additional quarter of a million flu cases could have been prevented, including nearly 6,000 hospitalisations and nearly 4,000 flu-related deaths.
Children from 24 months to less than 18 years should continue to be offered the quadrivalent live attenuated influenza vaccine (LAIV), Fluenz Tetra nasal spray.
THE ILLNESS
For most people, flu is a self-limiting illness, manifesting as fever, cough, sore throat, head ache, malaise and muscle and joint pains. It can be treated with rest at home and over-the-counter medication to alleviate symptoms. But in vulnerable people, flu can progress, and patients who present with shortness of breath, chest pain or confusion, indicative of pneumonia, and/or a significant exacerbation of an underlying medical condition such as heart, liver, lung or renal insufficiency or diabetes, will usually need to be referred for assessment and treatment in hospital.
CONCLUSION
Practice nurses are the lynch pin of the seasonal flu vaccination campaign, and without your hard work, the campaign will flop, with potentially disastrous consequences in the event of a major flu outbreak. We haven’t had a significant epidemic since the winter of 2011-12, but flu is unpredictable and who knows if we are in for another bad year?
Related articles
View all Articles