Practice Nurse Bite-Sized Learning: Understanding hypertriglyceridemia
MICHAELA NUTTALL RGN MSc, Founder & Director, Learn With Nurses
MICHAELA NUTTALL RGN MSc, Founder & Director, Learn With Nurses
JOANNE HAWS RN MSc, Clinical Director, Learn With Nurses
Practice Nurse 2024;54(1):8-9
Triglycerides (TRGs) are a main source of energy for the body and are made in the liver and from diet. However, raised TRGs can cause serious health problems
INTRODUCTION
Triglycerides (TRG) are a combination of:
- Three fatty acids: saturated fat, unsaturated fat or both
- Glycerol, a form of glucose
TRGs are a main source of energy for the body and are made in the liver and from diet. However, raised TRGs can cause serious health problems.
WHAT’S THE PROBLEM?
Hypertriglyceridemia (HTG) is commonly encountered in clinical practice, and the overall prevalence ranges from 10% to 25% in the adult population. Mild-to-moderate HTG is associated with an increased risk of atherosclerotic cardiovascular disease, while severe HTG may cause acute pancreatitis.1
HTG can have primary causes, i.e. genetic, or secondary causes such as:
Lifestyle:
- A sedentary lifestyle
- An unhealthy diet
- Alcohol
Medical conditions:
- Kidney disease
- Non alcoholic fatty liver disease
- Gout
- Pregnancy
- An under-active thyroid.
Medications:
- Some diuretics
- Steroids
- Oral oestrogen therapy
- Retinoids
- Retrovirals
DETECTION
Often, there are no symptoms of mild-moderate HTG. However, severe HTG triglycerides may have signs and symptoms such as pain in the mid-epigastric, chest, or back regions; nausea, vomiting, dyspnoea, xanthomas, corneal arcus or xanthelasmas. Usually, detection occurs when reviewing a lipid blood test.
DIAGNOSIS
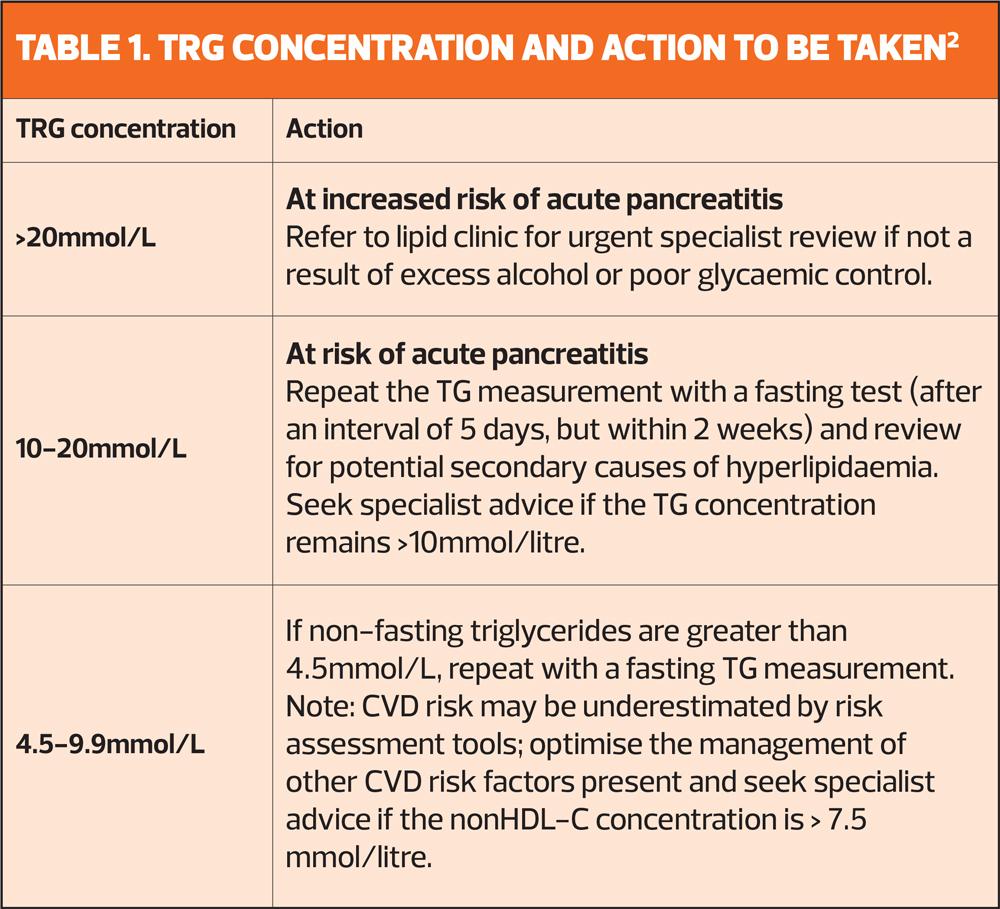
Table 1 shows the action that needs to be taken following a venous blood sample (either random or fasting). Depending on the levels diagnosis is made in primary or secondary care.
MANAGEMENT
Management depends on the severity of HTG. For those managed in primary care, before being started on a statin check:
- Smoking status
- Alcohol consumption
- Blood pressure
- BMI
- Full lipid profile
- Diabetes status
- Renal function
- Transaminase level
- Thyroid-stimulating hormone level in people with symptoms of underactive or overactive thyroid.
Lifestyle is often key in helping to manage TRG.
- Reach and maintain a healthy body weight
- Exercise regularly
- Cut down on saturated fats and replace these with unsaturated fats such as oily fish.
- Cut down on added sugars in food and drinks
- Drink alcohol in moderation, if at all.
REVIEW
- Measure liver transaminase and full lipid profile at 2 to 3 months after starting or changing lipid-lowering treatment.
- Measure liver transaminase at 12 months, but not again unless clinically indicated.
- Medication review including adherence
- Review of CVD risk factors and any support required
- Review of overall health and wellbeing, including mental health
References
1. BMJ Best Practice. Hypertriglyceridaemia; last updated June 2023. https://bestpractice.bmj.com/topics/en-gb/146
2. NICE NG238. Cardiovascular disease: risk assessment and reduction, including lipid modification; 14 December 2023. https://www.nice.org.uk/guidance/ng238/resources/cardiovascular-disease-risk-assessment-and-reduction-including-lipid-modification-pdf-66143902851781
Related articles
View all Articles